You've probably tried generic wellness advice that didn't work for your unique body. Perhaps you felt frustrated seeing "normal" blood test results while still experiencing fatigue, brain fog, or stubborn weight issues. Personalised wellness optimisation using blood biomarkers offers a targeted approach that goes beyond standard reference ranges. This guide walks you through the complete process: selecting appropriate tests, interpreting results using optimal ranges, implementing lifestyle changes, and monitoring progress to achieve sustainable health improvements tailored specifically to you.
Table of Contents
- Preparing For Wellness Optimisation: Defining Goals And Choosing Tests
- Interpreting Blood Test Results: Beyond UK Reference Ranges
- Implementing Lifestyle Changes Based On Biomarker Insights
- Monitoring Progress And Understanding Biomarker Trends
- Explore Personalised Wellness Solutions With ClearUp
- FAQ
Key takeaways
| Point | Details |
|---|---|
| Goal-driven testing | Start by defining your health objectives and selecting blood tests covering essential biomarkers like lipids, thyroid, vitamins, and inflammation markers. |
| Optimal vs reference ranges | UK reference ranges identify general health, but optimal ranges for longevity are stricter and better guide wellness goals. |
| Personalised interventions | Translate biomarker insights into targeted lifestyle changes focusing on nutrition, supplements, exercise, and sleep for your specific deficiencies. |
| Regular monitoring | Re-test key biomarkers every 3 to 6 months to track trends, verify intervention effectiveness, and adjust your wellness plan accordingly. |
Preparing for wellness optimisation: defining goals and choosing tests
Before requesting blood tests, clarify what you want to achieve. Are you addressing persistent fatigue, managing weight, supporting hormonal balance, or preventing chronic disease based on family history? Your symptoms and wellness ambitions determine which biomarkers matter most. Someone experiencing low energy might prioritise thyroid function, iron status, and vitamin B12, whilst someone focused on cardiovascular health would emphasise lipid profiles and inflammatory markers. Write down your top three health concerns to guide test selection.
Comprehensive wellness testing typically includes several key panels. A full blood count reveals red and white cell status, indicating anaemia or immune function. Liver and kidney function tests assess detoxification and filtration capacity. Lipid panels measure cholesterol fractions critical for cardiovascular risk. Thyroid tests (TSH, T3, T4) evaluate metabolism regulation. Hormone panels check testosterone, oestrogen, and cortisol depending on your age and symptoms. Vitamin levels (D, B12, folate, iron/ferritin) identify common deficiencies affecting energy and immunity. Finally, inflammatory markers like high-sensitivity C-reactive protein signal chronic inflammation linked to numerous diseases.
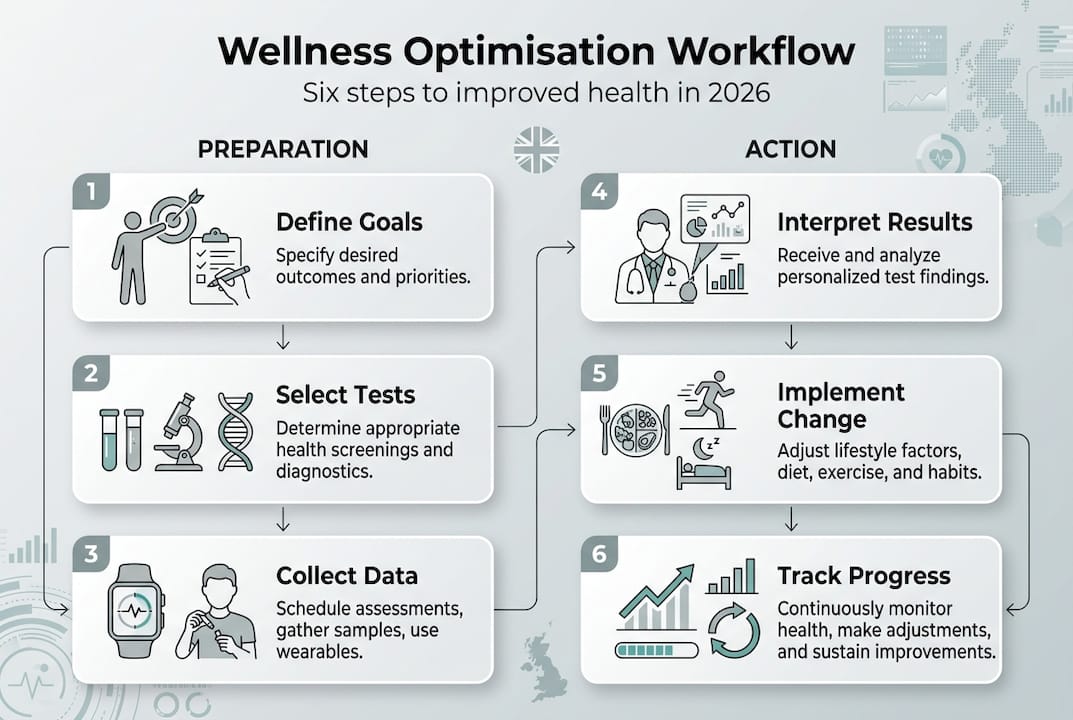
The 6-step workflow provides a structured approach: identify health objectives, select appropriate tests, interpret results against optimal ranges, implement targeted interventions, re-test after 3 to 6 months, and adjust based on progress. This cyclical process ensures continuous refinement rather than one-off testing. Most UK adults benefit from starting with a comprehensive metabolic panel covering the biomarkers mentioned above, then adding specialised tests based on initial findings or specific concerns.
Pro Tip: Request copies of all blood test results from your GP, even if told they're "normal." You'll need the actual numbers to compare against optimal ranges and track trends over time, which standard NHS feedback often doesn't provide in sufficient detail.
When booking tests, consider timing factors. Fasting tests (glucose, lipids) require 8 to 12 hours without food. Hormone tests may need specific cycle timing for menstruating individuals. Vitamin D testing is most informative at the end of winter when levels are typically lowest. Schedule your initial comprehensive panel, then use the same testing conditions for follow-ups to ensure valid comparisons.
Interpreting blood test results: beyond UK reference ranges
Receiving blood test results marked "normal" doesn't necessarily mean optimal for longevity and wellness. UK reference ranges reflect the middle 95% of the tested population, which includes many people with suboptimal health. These ranges identify disease states but miss opportunities for prevention and optimisation. Understanding the difference between reference and optimal ranges transforms how you approach wellness.
Consider fasting glucose as an example. The UK reference range allows up to 5.5 mmol/L (99 mg/dL) as normal, yet research suggests optimal fasting glucose sits between 3.9 to 4.7 mmol/L (70 to 85 mg/dL) for metabolic health and longevity. Similarly, ferritin reference ranges span 15 to 300 µg/L, but optimal function for energy and thyroid health occurs between 50 to 100 µg/L. HbA1c below 42 mmol/mol (6.0%) is considered non-diabetic, whilst optimal sits below 37 mmol/mol (5.5%) to minimise glycation and inflammation.
| Biomarker | UK Reference Range | Optimal Range for Wellness | | --- | --- | | Fasting Glucose | 3.0-5.5 mmol/L | 3.9-4.7 mmol/L | | HbA1c | Below 42 mmol/mol | Below 37 mmol/mol | | Ferritin | 15-300 µg/L | 50-100 µg/L | | Vitamin D | Above 25 nmol/L | 75-125 nmol/L | | TSH | 0.4-4.0 mIU/L | 1.0-2.0 mIU/L |
Context matters enormously when interpreting lab results. Age, sex, medications, recent illness, and lifestyle factors all influence biomarker values. A 25-year-old athlete's optimal ranges differ from a 65-year-old's. Menstruating individuals typically have lower ferritin than post-menopausal women or men. Statin medications alter lipid interpretation. Recent intense exercise can temporarily elevate liver enzymes and creatine kinase. Always consider your full health picture rather than isolated numbers.
Pro Tip: Track trends across multiple tests rather than obsessing over single values. A ferritin level dropping from 80 to 45 µg/L over six months signals a concerning trend requiring investigation, even though both values sit within reference ranges. Trends reveal developing issues before they become clinically significant.
Professional guidance proves invaluable here. Whilst you can research optimal ranges, healthcare practitioners trained in functional medicine or preventative health can integrate your complete clinical picture, identify subtle patterns, and recommend appropriate interventions. They'll also know when borderline results warrant further investigation versus lifestyle modification. Self-interpretation risks missing important nuances or creating unnecessary anxiety over minor variations.
Implementing lifestyle changes based on biomarker insights
Once you've identified biomarkers outside optimal ranges, translate those insights into targeted lifestyle interventions. Personalisation is key. Rather than following generic wellness advice, you're addressing your body's specific needs revealed through testing. This precision approach delivers better results with less wasted effort. Start by prioritising two to three key biomarkers requiring attention, avoiding the overwhelm of changing everything simultaneously.
![]()
Vitamin supplementation addresses deficiencies directly. Low vitamin D (below 75 nmol/L) responds well to 2,000 to 4,000 IU daily supplementation, with re-testing after three months to confirm adequate dosing. B12 deficiency under 400 pg/mL improves with sublingual methylcobalamin or, if severe, GP-supervised injections. Low ferritin benefits from iron supplementation taken with vitamin C for enhanced absorption, though investigate underlying causes like heavy menstrual bleeding or poor dietary intake. Magnesium supplementation (300 to 400 mg daily) supports numerous biochemical processes and often improves sleep quality when levels are suboptimal.
Dietary modifications target metabolic markers effectively. Elevated fasting glucose or HbA1c responds to reduced refined carbohydrate intake, increased fibre consumption, and strategic meal timing. High LDL cholesterol improves with increased soluble fibre from oats, beans, and vegetables, whilst reducing saturated fat intake. Elevated triglycerides respond particularly well to cutting added sugars and alcohol. Anti-inflammatory diets rich in omega-3 fatty acids, colourful vegetables, and polyphenols from berries and green tea help lower high-sensitivity C-reactive protein.
Hormone optimisation requires attention to stress management and sleep quality. Elevated cortisol patterns benefit from mindfulness practices, regular relaxation techniques, and addressing chronic stressors. Low testosterone in men often improves with resistance training, adequate sleep (7 to 9 hours), and maintaining healthy body composition. Thyroid function optimisation may require addressing nutrient cofactors like selenium, zinc, and iodine, though always work with healthcare providers when thyroid issues are present.
Pro Tip: Use a 12-week intervention cycle as your baseline timeframe. Lipid markers typically show measurable changes within 6 to 8 weeks, whilst HbA1c requires approximately 3 months to reflect dietary modifications. This prevents premature judgement of intervention effectiveness.
Implement changes gradually for sustainability. Adding one new habit weekly proves more effective than overhauling your entire lifestyle overnight. Start with the highest-impact intervention for your priority biomarker. If low vitamin D is your main concern, begin supplementation immediately. If elevated glucose is the issue, start by eliminating sugary drinks and refined carbohydrates. Once the first change becomes habitual (usually 3 to 4 weeks), layer in the next intervention. This approach builds lasting behaviour change rather than temporary motivation-driven efforts.
Track your interventions systematically. Document which supplements you're taking, dietary changes you've made, exercise modifications, and sleep improvements. This record proves invaluable when reviewing your next blood test results, allowing you to identify which interventions drove specific biomarker improvements. Many people see positive changes but forget exactly what they implemented, making it difficult to maintain successful strategies long-term.
Monitoring progress and understanding biomarker trends
Wellness optimisation is an iterative process requiring regular monitoring to verify intervention effectiveness and detect emerging issues early. Re-testing key biomarkers every 3 to 6 months provides the feedback loop necessary for continuous improvement. This frequency allows sufficient time for lifestyle changes to impact biomarkers whilst catching problems before they progress. Annual testing, whilst better than nothing, misses opportunities for timely adjustments.
Focus re-testing on biomarkers you're actively working to improve plus a few core health indicators. If you implemented interventions for low vitamin D and elevated HbA1c, definitely re-test those markers. Additionally, include a basic metabolic panel and lipid profile to ensure other markers haven't shifted unexpectedly. You needn't repeat every test from your initial comprehensive panel unless new symptoms emerge or previous results suggested monitoring specific markers.
Trend analysis reveals far more than isolated values. A single test showing ferritin at 45 µg/L might not concern you, but seeing a progression from 80 to 65 to 45 over 18 months indicates iron depletion requiring investigation. Similarly, gradually rising fasting glucose from 4.4 to 4.8 to 5.2 mmol/L over two years signals developing insulin resistance, even though all values sit within reference ranges. Early biomarker shifts can predict diseases 5 to 7 years before clinical diagnosis, making trend monitoring invaluable for prevention.
| Monitoring Approach | Timeframe | Best For | | --- | --- | | Quarterly testing | Every 3 months | Active intervention periods, metabolic issues | | Biannual testing | Every 6 months | Maintenance phase, hormone monitoring | | Annual comprehensive | Once yearly | Broad health screening, new baseline |
Emerging biomarker models offer sophisticated wellness insights beyond traditional markers. Seven-biomarker ageing clocks using albumin, creatinine, glucose, C-reactive protein, lymphocyte percentage, mean cell volume, and red cell distribution width predict biological age and mortality risk. The Proteomic Health Age Score (PHAS) analyses plasma proteins to forecast cardiometabolic disease risk years in advance. Whilst these advanced tools aren't yet standard practice, they represent the future of preventative wellness monitoring.
Adjust your wellness plan based on evolving data. If vitamin D supplementation brought your levels from 45 to 95 nmol/L, you might reduce dosage to a maintenance level rather than continuing high-dose supplementation. If dietary changes successfully lowered HbA1c from 40 to 35 mmol/mol, maintain those habits whilst perhaps focusing attention on a different biomarker needing optimisation. If interventions failed to move a stubborn marker, reassess your approach or seek professional guidance for alternative strategies.
Pro Tip: Photograph or scan all test results and store them in a dedicated folder on your phone or computer. This creates a portable health record you can share with any healthcare provider and easily reference when making wellness decisions. Many NHS systems don't provide long-term access to historical results.
Celebrate improvements whilst maintaining perspective. Biomarker optimisation is a long game, not a quick fix. Some markers respond rapidly to intervention, whilst others require months of consistent effort. Hormonal changes can take 6 to 12 months to stabilise. Inflammatory markers may fluctuate with stress, illness, or sleep quality. Focus on overall trajectory rather than minor fluctuations between tests. The goal is sustained wellness, not perfect numbers at every test.
Explore personalised wellness solutions with ClearUp
Transforming blood test insights into lasting wellness improvements requires the right tools and support. ClearUp lab testing services provide comprehensive biomarker analysis tailored to your specific health goals, going beyond standard NHS panels to include markers crucial for optimisation. You'll receive detailed results with context about what each biomarker means for your wellness journey.
Access personalised nutrition support that translates your blood test findings into specific dietary recommendations addressing your unique deficiencies and imbalances. Rather than generic meal plans, you'll receive targeted guidance based on your actual biomarker data. Supplement recommendations are similarly personalised, ensuring you're only taking what your body genuinely needs. Track your improvements with ClearUp's progress monitoring tools, visualising biomarker trends over time and celebrating milestones as you optimise your health. Let ClearUp guide you through each step of your wellness journey with professional support.
FAQ
What blood tests are essential for wellness optimisation?
Comprehensive wellness testing typically includes full blood count, lipid panel, liver and kidney function, thyroid markers (TSH, T3, T4), key vitamins (D, B12, folate, iron/ferritin), and inflammatory markers like high-sensitivity C-reactive protein. Choose essential wellness blood tests based on your personal health goals, symptoms, and family history. Someone focused on energy might prioritise thyroid and iron, whilst cardiovascular prevention emphasises lipids and inflammation markers.
How often should I re-test my blood biomarkers when optimising wellness?
Typically every 3 to 6 months depending on which biomarkers you're targeting and how aggressively you're intervening. This timeframe allows sufficient time for lifestyle changes to impact markers like lipids (6 to 8 weeks) and HbA1c (approximately 3 months) whilst providing timely feedback to adjust your approach. Annual testing works for maintenance phases, but active optimisation benefits from more frequent monitoring.
Why is professional interpretation important for my blood test results?
UK reference ranges are broad population averages that identify disease but miss optimal wellness targets. Professional lab interpretation considers your personal context including age, sex, symptoms, lifestyle factors, and longevity research to provide nuanced guidance. Practitioners trained in functional medicine can identify subtle patterns, recommend appropriate interventions, and determine when borderline results warrant further investigation versus lifestyle modification.
Can I optimise wellness using only NHS blood tests?
NHS tests provide valuable baseline data and cover many essential biomarkers for wellness optimisation. However, NHS testing typically focuses on disease diagnosis rather than optimal ranges, and some wellness-relevant markers like high-sensitivity C-reactive protein, comprehensive vitamin panels, or advanced lipid fractions may require private testing. You can certainly begin your wellness journey with NHS results, then selectively add private tests for markers your GP doesn't routinely check.
